In restorative oral surgery, bone grafting is essential, especially when patients don’t have enough bone mass for dental implants or other oral surgical procedures. Both patients and oral surgeons must comprehend the nuances of the healing process. This blog aims to provide insight into the parameters, timetable, and subtleties associated with oral bone graft healing. By examining the healing phases, possible issues, and strategies for fostering favorable outcomes, readers will understand what to anticipate from their bone grafting procedures. Come along as we explore the intriguing realm of oral bone graft recovery.
What Is an Oral Bone Graft?
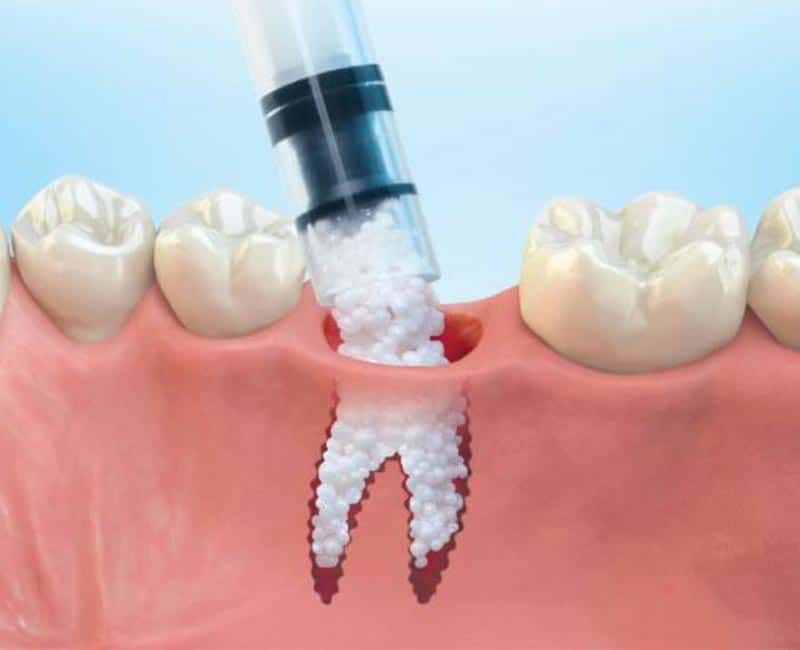
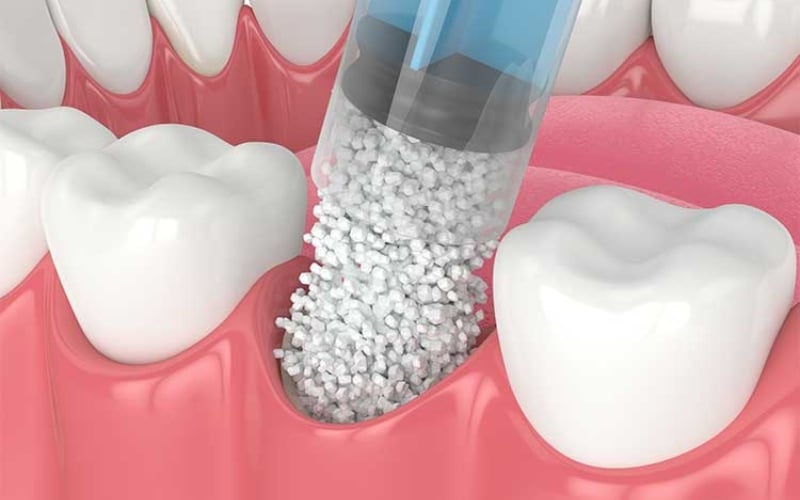
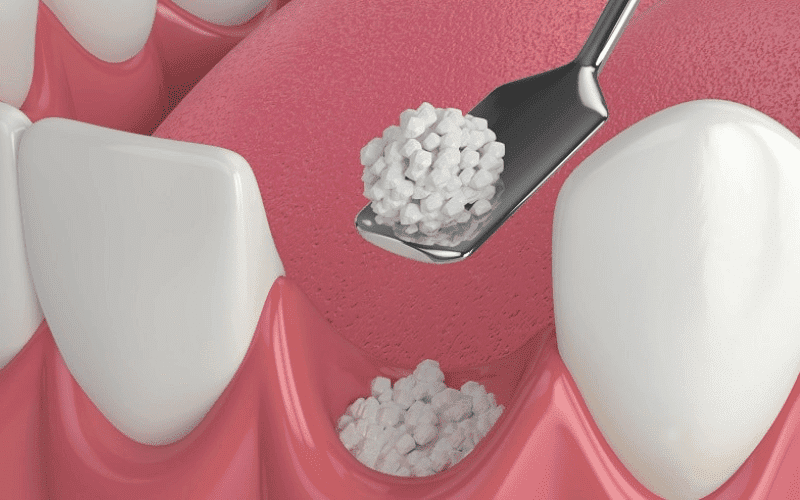
An oral bone graft is a surgical procedure that involves replacing missing or damaged bone in the jaw with material sourced from the patient’s body, a donor, or synthetic sources. This procedure commonly prepares the jawbone for dental implants by providing a sturdy foundation. It can also repair bone defects caused by trauma, disease, or tooth loss. The bone graft material acts as a scaffold, promoting the growth of new bone tissue over time. This process restores the jawbone’s strength, shape, and volume, facilitating various oral surgical procedures and improving overall oral health.
Types of bone graft materials
Bone graft materials used in oral surgical procedures can be classified into several categories:
1. Autografts: Bone tissue harvested from the patient’s own body, often from areas such as the chin, jaw, hip, or tibia. Autografts are considered the gold standard due to their compatibility and ability to promote natural bone growth.
2. Allografts: Bone tissue obtained from human donors, typically from cadavers. Allografts undergo rigorous processing to remove cellular components while retaining the bone’s structural properties. They serve as an alternative when autografts are not feasible.
3. Xenografts: Bone graft material from animals, commonly bovine (cow) or porcine (pig) sources. Xenografts are processed to remove antigenic components, making them biocompatible for human use. They provide a scaffold for new bone formation and are often used with other graft materials.
4. Synthetic grafts: Biocompatible materials designed to mimic the properties of natural bone. These include ceramics, calcium phosphate compounds, and bioactive glasses. Synthetic grafts offer precise control over composition and structure, promoting predictable bone regeneration.
5. Growth factors and bone substitutes: Biological agents such as recombinant human bone morphogenetic proteins (rhBMPs) or platelet-rich plasma (PRP) can be combined with other graft materials to enhance bone regeneration. These substances stimulate cellular activity and accelerate the healing process.
Each type of bone graft material has its advantages and considerations, and the choice depends on factors such as the patient’s medical history, the extent of bone loss, and the specific requirements of the oral surgical procedure.
Common reasons for needing a bone graft
1. Tooth extraction: After tooth removal, the surrounding bone may resorb over time, mainly if the extraction site is left untreated. A bone graft may be necessary to preserve bone volume and maintain the structural integrity of the jaw for future dental implant placement or aesthetic reasons in oral surgery.
2. Periodontal disease: Severe periodontitis can lead to bone loss around the teeth, compromising their stability and affecting oral function. Bone grafting may be required to regenerate lost bone tissue and support the teeth or oral implants.
3. Trauma or injury: Facial trauma, such as fractures or accidents involving the jawbone, can result in bone loss or defects. Bone grafts may be used to reconstruct and restore the damaged bone to its original form and function.
4. Congenital disabilities: Some individuals may be born with congenital conditions affecting the development of the jawbone, resulting in abnormalities or deficiencies. Bone grafting can help correct these defects and improve the overall structure and function of the jaw.
5. Sinus augmentation: In cases where the height of the bone in the upper jaw is insufficient for dental implant placement, a sinus lift or sinus augmentation procedure may be performed. This involves lifting the sinus membrane and placing bone graft material in the space created to promote new bone formation, providing adequate support for dental implants in the posterior maxilla.
The Healing Process
A. Initial healing stages:
1. Blood clot formation: Immediately after bone graft surgery, a blood clot forms at the surgical site. This clot serves as a protective barrier and initiates the healing process by providing a framework for tissue regeneration.
2. Inflammation and swelling: In the first few days following surgery, inflammation and swelling are common reactions as the body responds to the trauma of the procedure. This inflammatory phase is crucial to the healing process, as it brings necessary nutrients and immune cells to the area to promote healing.
B. Bone formation:
1. Osteoblast activity: Within the first few weeks after surgery, specialized osteoblasts migrate to the bone graft site. These cells produce a new bone matrix, serving as the bone regeneration framework.
2. New bone formation: The bone graft material gradually incorporates with the surrounding bone tissue over the following months. Osteoblasts continue to deposit minerals onto the bone matrix, leading to the formation of new bone tissue.
C. Maturation and remodelling:
1. Strengthening of new bone: As the bone graft heals and matures, the newly formed bone tissue becomes more organized and dense. This process, known as bone remodelling, involves the removal of old bone by cells called osteoclasts and the deposition of new bone by osteoblasts, resulting in more robust and more resilient bone.
2. Integration with existing bone: Over time, the bone graft material fully integrates with the surrounding bone tissue, creating a seamless transition between the graft and the native bone. This integration is essential for the long-term success and stability of dental implants or other oral prosthetics placed in the area.
Factors Affecting Healing Time
A. Type and size of bone graft:
1. Graft type: Different bone graft materials have varying rates of resorption and integration. Autografts, for example, may have a faster healing time as they are the patient’s tissue. Synthetic grafts may take longer to integrate with existing bone.
2. Graft size: The extent and volume of the bone graft also influence healing time. Larger grafts may require more time for complete vascularisation and integration.
B. Patient’s overall health:
1. Systemic health: Overall, health plays a significant role in the body’s ability to heal. Conditions such as diabetes or compromised immune function may slow down the healing process.
2. Nutritional status: Adequate nutrition, particularly with essential vitamins and minerals like calcium and vitamin D, is crucial for bone health and can impact the rate of bone graft healing.
C. Oral hygiene and post-operative care:
1. Infection prevention: Strict adherence to post-operative care instructions, including proper oral hygiene practices, can prevent infections that might compromise healing.
2. Medication compliance: Following prescribed medications, such as antibiotics or pain relievers, can aid in controlling inflammation and promoting optimal healing.
D. Presence of underlying conditions:
1. Smoking: Tobacco use can significantly delay the healing process by restricting blood flow and impairing tissue oxygenation. Smokers may experience a higher risk of complications and slower bone graft integration.
2. Osteoporosis: Patients with osteoporosis may have compromised bone density, affecting the success of bone grafts. Additional measures may be required to support the healing process in these individuals.
Understanding and managing these factors is crucial for oral surgeons and patients to optimize the healing time and ensure successful outcomes following a bone graft procedure.
Timeline of Healing
A. Short-term healing (first few weeks):
1. Initial recovery: In the first few days after surgery, patients may experience swelling, bruising, and discomfort at the graft site. Pain and swelling typically peak within 48 to 72 hours post-surgery.
2. Blood clot formation: Within the first week, the blood clot at the surgical site begins to organize and initiate the healing process. The clot serves as a scaffold for tissue regeneration and protects the underlying bone graft.
3. Early bone formation: Osteoblasts migrate to the graft site and lay down the initial bone matrix. This process begins within the first week and continues throughout the short-term healing phase.
B. Mid-term healing (several months):
1. New bone formation: Over the next few weeks to months, the bone graft undergoes osteogenesis, where new bone tissue forms and replaces the graft material. This process is characterized by the deposition of minerals and the gradual maturation of the bone tissue.
2. Vascularization: Blood vessels gradually grow into the newly formed bone tissue, providing oxygen and nutrients essential for bone healing and remodelling.
3. Graft integration: The bone graft material integrates with the surrounding bone tissue, forming a stable and functional union. This process typically occurs within three to six months after surgery, depending on the Type and size of the graft.
C. Long-term healing (up to a year or more):
1. Maturation and remodelling: The newly formed bone undergoes maturation and remodelling over several months to a year or more. This involves the continuous turnover of bone tissue, with old bone being resorbed by osteoclasts and replaced by new bone laid down by osteoblasts.
2. Functional restoration: As the bone graft fully integrates and remodels, the jawbone’s strength, volume, and density are restored. This process is essential for the long-term success and stability of dental implants or other oral prosthetics placed in the area.
3. Follow-up evaluations: ChatGPT said:
Patients typically undergo periodic appointments with their oral surgeons to monitor healing progress, assess graft integration, and plan for additional oral procedures if needed.
Tips for Promoting Healing
A. Following post-operative instructions:
1. Take prescribed medications: Follow the instructions provided by your oral surgeon. regarding medications such as antibiotics or pain relievers to manage discomfort and prevent infections.
2. Attend follow-up appointments: Attend all scheduled follow-up appointments to monitor healing progress and promptly address any concerns or complications.
3. Rest and recovery: Follow recommendations for rest and limited activity to allow your body to heal correctly.
B. Maintaining good oral hygiene:
1. Gentle oral care: Practice gentle oral hygiene as your oral surgeon instructs to avoid disrupting the healing process.. Use a soft-bristled toothbrush and be cautious around the surgical site.
2. Rinse with a saline solution: Rinse your mouth with a saline solution as directed to keep the surgical site clean and promote healing.
3. Avoid tobacco and alcohol: Refrain from smoking and consuming alcohol, as they can delay healing and increase the risk of complications.
C. Eating a healthy diet:
1. Nutrient-rich foods: Consume a balanced diet of vitamins, minerals, and protein to support healing. Include foods high in calcium, vitamin D, and protein essential for bone health.
2. Hydration: Drink plenty of water to stay hydrated, which aids in tissue repair and promotes overall health.
3. Avoid hard or crunchy foods: Avoid hard or crunchy foods that may irritate the surgical site or dislodge the blood clot.
D. Avoiding activities that may disrupt healing:
1. Avoid strenuous activities: Refrain from strenuous physical activities or exercise that may increase blood pressure or strain the surgical site.
2. Avoid chewing on the surgical site: Avoid chewing on the side of the mouth where the bone graft was placed to prevent trauma to the area.
3. Be cautious with oral appliances: If you wear removable oral appliances, such as dentures or retainers, follow your oral surgeon’s instructions regarding their use during the healing period.
Following these tips and guidelines can help promote optimal healing following a bone graft procedure and achieve successful outcomes.
Final Words!
In conclusion, understanding the nuances of bone grafting is paramount for successful outcomes. We’ve explored vital points, from initial healing to long-term recovery, emphasizing the significance of following post-operative care. Patience is crucial during the process, and we should recognise that healing takes time. At Beverly Hills Oral and Facial Surgeon, we are always committed to providing you with the best bone grafting treatment in Beverly Hills. Relax; you can count on us as your journey is in expert hands. As you embark on this transformative experience, remain steadfast; your restored oral health is worth the wait. Schedule your consultation today, and let your journey to a confident smile begin!